Abdominoplasty (Tummy Tuck)
A Tummy Tuck or Abdominoplasty may help to restore your body shape for those bothered by a large fat deposit and loose skin in the abdomen or stomach area.
A Tummy Tuck or Abdominoplasty may help to restore your body shape for those bothered by a large fat deposit and loose skin in the abdomen or stomach area.
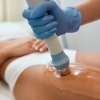
Acoustic Wave Therapy (also called sound, pressure or shock wave therapy) has been shown to safely reduce the appearance of cellulite and improve the tone, elasticity and firmness of the skin.

Alevere therapy® is a comprehensive weight loss and body contouring programme that consists of four different techniques: ultrasound therapy, connective tissue massage, medical diet and stabilisation.
The Alkaline Wash system, available through the Danne Montague King product range is designed to reduce fine, downy hair on the face and other parts of the body.
The need to achieve significant weight loss, due to obesity, is a growing problem. For those seeking medical intervention to help them through this journey, there are medically-led, anti-obesity solutions such as prescribed weight loss medication or slimming pills. These are available through private clinics.

Bariatric or weight-loss surgery for the treatment of obesity uses gastric band or gastric bypass operations to restrict the amount of calories a person can consume and help them to lose weight.

Bio-Identical Hormone Replacement Therapy (BHRT) is an alternative treatment to the synthetic hormones, used in conventional Hormone Replacement Therapies (HRT).
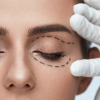
Upper and lower eyelid surgery or Blepharoplasties can help restore a more youthful appearance by tightening droopy or hooded eyelids and removing or moving fatty pouches beneath the eyes.
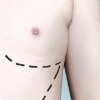
Body implants, (e.g. pectoral, testicular, calf and buttock) are used to correct defects, which have existed since birth, or to put right tissue loss, which has occurred through injury or disease.
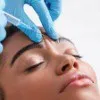
Botulinum toxin type A, know by the brand names Botox (Vistabel), Dysport (Azzalure) and Xeomin (Bocouture), is a naturally occurring protein produced by the bacterium clostridium botulinum. It is licensed as a prescription only medicine and can be used to treat wrinkles like frown lines and crow`s feet as well as hyperhidrosis or excessive sweating. As a prescription only medicine, it requires a face-to-face consultation to determine your suitability for treatment.
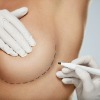
Breast implants, enhancement, enlargement or augmentation is one of the most popular cosmetic surgery procedures in the UK. This section contains more info on implant cost, risks & UK clinics.
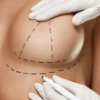
A breast lift or Mastopexy can improve the appearance of the breasts in several ways. It raises the breast tissue, repositions the nipple and areola and enhances breast shape.
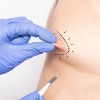
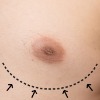
There are several different cosmetic procedures used for the enhancement or reduction of the nipple or brownish area around the breast (areola). These treatments are available for both men and women.
Gynaecomastia is a medical term that comes from the Greek meaning female-like-breasts. This condition occurs when firm breast tissue forms in men. Surgery can reduce the size of these breasts.

Breast reduction or a reduction mammaplasty is an operation that removes fat, tissue, and skin from the breasts to reduce and reshape them. Afterwards, the breasts should have a more youthful shape.

The muscles under the skin of the forehead that cause lines can be released to help create a smoother brow. This can be performed using an endoscopic forehead or brow lift.
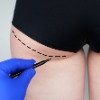
There are several different procedures that can be used to improve the buttock shape and appearance. The buttock can be lifted, reshaped with liposuction or added to with implants or fat.
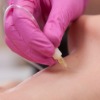
Carboxytherapy, also referred to as carbon dioxide therapy or CDT is becoming more widely used within UK aesthetic clinics for skin rejuvenation and cellulite reduction.

Cell Therapies like Recell® use the patient’s own skin cells to repair and rejuvenate the skin; treating lines and wrinkles, scars and burns.
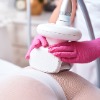
Cellulite is often referred to as looking like “orange peel” on the skin. Endermologie® is the world’s first patented mechanical cellulite treatment technology to be approved by the FDA.
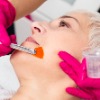
The use of chemical peels to soften and improve the appearance of skin dates back to the ancient Egyptians. Today, scientists have identified numerous forms of acid which can be used to treat skin.

Cosmetic skin camouflage is the art of concealing a discolouration, blemish or scar with the application of specialist camouflage creams that are matched to the surrounding skin tones.
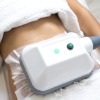
Cryolipolysis is a non-invasive fat removal procedure. It involves the cooling of subcutaneous fat cells, which induces lipolysis, the breaking down of the fat cells, without damaging any of the surrounding tissues or the skin.

Focused Cold Therapy, generically known as cryoneuromodulation is designed to improve the appearance of fine lines and facial wrinkles using highly pressurised nitrous oxide, as a toxin free alternative to botulinum toxins.
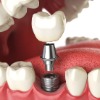
Dental implants are a new way of replacing single, or a whole set of completely missing teeth, and are a real alternative to dentures for people who have a lot of missing teeth.

Veneers offer one of the best cosmetic dentistry options for people wanting whiter teeth than bleaching can achieve or who want to camouflage spaces between “gappy” teeth and/or overcrowded teeth.
Dermabrasion is a surgical procedure which aims to “resurface” the skin. It uses a machine to remove the outer layer of the skin or epidermis and then the top third part of the dermis of the skin.

Looking to restore volume, smooth wrinkles, or contour your face? This comprehensive UK-based guide to dermal fillers explains everything you need to know.
Advanced Cosmetic Procedures (ACP) is a new name for "Advanced Electrolysis". ACP uses either Short Wave Diathermy or Blend to treat unwanted skin blemishes, such as warts, skin tags, moles and other benign growths, as well as thread veins and vascular conditions with no mark left on the skin.
The first recorded use of electricity for epilation or hair removal was in 1875. Currently, needle-type electrolysis is the only method which can guarantee permanent hair removal. Advanced techniques are used to also remove lumps and bumps such as moles and warts.
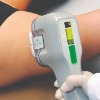
Hyperhidrosis is a medical condition whereby a person has abnormally increased or excessive perspiration or sweating. miraDry is the first and only device cleared by the U.S. FDA for the treatment of excessive underarm sweat.
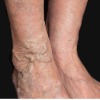
Endovenous Laser Ablation (EVLA), also referred to as Endovenous Laser Treatment (EVLT) is a minimally invasive method of treating varicose veins.

A face lift or rhytidectomy can reduce the appearance of loose skin and wrinkles around the cheeks and neck, by tightening the muscles and removing excess skin and fat, restoring a more youthful look.

Facial implants for areas such as the cheek or chin are used to correct defects, which have existed since birth, or by cosmetic surgeons for malarplasty (reshaping of the cheeks and jaw line)

Fat transfer, fat transplantation or microlipoinjection involves the collection of fat via liposuction for re-injection into other areas of the face and body.
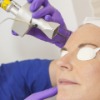
Unlike ablative and non-ablative lasers Fractional Laser Skin Resurfacing (Fractional Photothermolysis) only damages small zones within a target area, causing fractional trauma and quicker recovery.

Chin Surgery or Genioplasty refers to cosmetic surgery operations that aim to improve the appearance of a person`s chin.
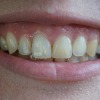
Gummy smiles are a common problem, caused by overgrowth of the gum tissue that then covers the teeth. This can be easily corrected with a procedure known as a cosmetic gum lifting or contouring.

The drugs that are currently medically approved treatments for hair loss are Minoxidil, first discovered in the 1970’s and Propecia which has been used since the 1990’s.
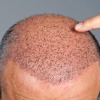
Hair transplant or hair restoration surgery for hair loss involves the surgical transplantation of small hair grafts, which produce quite natural looking results and are often indistinguishable from normal hair.

Book your HydraFacial today! Find the best HydraFacial clinics near you. This rejuvenating treatment cleanses, hydrates, and revitalizes for glowing skin!

Infra Red Laser Skin Tightening, currently available in the UK using the Titan device, is the latest, minimally invasive way to tighten skin and reverse the signs of ageing.
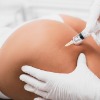
Injectable Body Contouring currently available using Macrolane, is the first body shaping and volume restoration product which uses hyaluronic acid, a natural component of our own bodies.
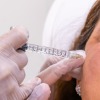
Unlike dermal fillers which are aimed at mechanically filling wrinkles, folds and skin depressions, tissue stimulators are injectable products which cause a biological reaction in the tissue.

Intravenous or IV Nutritional Therapy delivers a controlled dose of electrolytes, vitamins, minerals and other nutrients directly into your body intravenously or directly into your bloodstream through your vein.

There are various alternatives to traditional metal braces now available, including clear aligners and lingual braces.
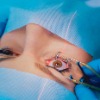
LASEK (Laser Assisted Sub-Epithelial Keratectomy) is a laser eye surgery for the correction of vision conditions. LASEK is specifically used to correct astigmatism, hyperopia (long or far sightedness), and myopia (short or near sightedness).
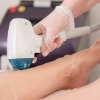
Many different types of Laser and IPL, or LHE devices have been developed to remove body hair to a significant degree. This section contains more info on treatment cost, side effects and UK clinics.
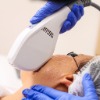
Laser, Intense Pulsed Light (IPL), Light Heat Energy (LHE) and Light Emitting Diode (LED)technologies have been developed to treat a variety of skin problems including sun damage effects and wrinkles.
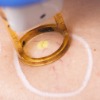
Laser and light technologies have been developed to treat people with a variety of different skin problems including pigmented (skin colour, birthmark) and vascular (vein) problems.
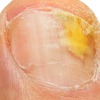
Fungal nail infection, or onychomycosis, is very common. It is caused by a fungus, similar to the one that causes Athlete`s foot, which attacks the fingernails or more commonly toenails. Laser treatment is effective for fungal nail infections.

On its own low-level laser hair loss therapy has been shown to be effective in improving hair thickness, but is often combined with proven hair loss drugs for a full hair loss treatment program.
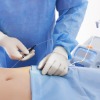
Laser Lipolysis, currently available using mainly the Smartlipo laser, is a minimally invasive way of removing small localised fat deposits which are resistant to diet or exercise.
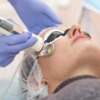
Laser skin resurfacing involves the removal of the outer layer of the skin using an ablative laser to improve the appearance of sun damaged skin or acne scars, lines, wrinkles, and pigment changes.
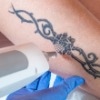
The removal of tattoos using lasers has been carried out for over 20 years; the use of certain lasers, Q-Switched Ruby and Nd:YAG, have become the preferred method for tattoo removal treatment.

LASIK (Laser-Assisted in Situ Keratomileusis) is a laser eye surgery used to correct and enhance the vision of long-sighted (hyperopic) and short-sighted (myopic) people, as well as those with astigmatism.

The use of Light Emitting Diodes (LEDs), red, yellow and blue light sources for the treatment of acne and for skin rejuvenation.

Until recently, topical preparations and oral medications, including antibiotics, have been used almost exclusively to combat acne. Now laser & light-based technologies and photodynamic therapy had been shown to improve acne.

Lip implants using natural or man-made products are used as a more permanent cosmetic procedure than dermal fillers or fat transfer, to improve the shape and size of the lips.
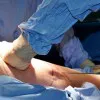
Liposuction (also called lipoplasty, liposculpture or lipectomy) is a surgical technique for removing specific areas of stubborn fat that do not respond to a healthy diet and regular exercise.
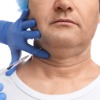
Lipotherapy or Injection Lipolysis treatment involves the use of an injectable solution to break down stubborn areas of fat, which are then eliminated through the body`s own lymphatic system. Products include Aqualyx.
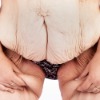
A lower body lift is part of a cosmetic surgery procedure called body contouring which is designed to remove large amounts of excess skin and fat from the stomach, hips, thighs, and back.
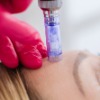
Medical Skin Needling, also referred to as Collagen Induction Therapy and Micro-Needling is aimed at stimulating the body’s own collagen production to reduce the appearance of fine lines and wrinkles.
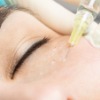
Mesotherapy is a medical technique used for the treatment of cosmetic conditions, including skin rejuvenation and improvement, hair regrowth, localised fat reduction and as a treatment for cellulite.
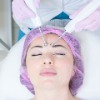
Micro-current therapy has been available in the UK since the early 90s with the introduction of the CACI (Computer Aided Cosmetology Instrument) which is known as the original non-surgical face lift. It can also be used to treat other areas of the body, such as mild lifting of the breast.

Microdermabrasion helps improve the texture and appearance of the skin using a stream of fine micro particles which partially removes the outermost layer of the skin and stimulates new cell growth.
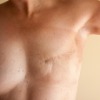
Reconstructive or medical micropigmentation attempts to correct or camouflage birth defects, repair disfigurement from accident or illness and simulate the areola after mastectomy.

The specialist techniques used to create semi-permanent make-up are often referred to as micropigmentation and provide an alternative to cosmetic pencils applied to the eyebrows, eyelids and lips.
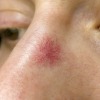
The use of high frequency microwave energy has become available in the UK for the treatment of thread veins and other skin lesions through thermocoagulation. An example of this is Veinwave or Thermavein.

No-needle mesotherapy (e.g. Eporex™ & Acthyderm®) seek to encourage the penetration of topically applied active ingredients through the skin using mild electric currents to treat ageing & reduce fat.
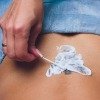
Non-Laser options for the removal of unwanted tattoos.

Non-surgical hair replacement systems, also known as hair bonding or hair integration allow you to sleep, shower, swim and carry on with your life as if you had your own hair.

The availability of non-surgical options for vulvo-vaginal rejuvenation to target both cosmetic and practical concerns such as labial remodelling of the outer vaginal lips, vaginal tightening for great sexual satisfaction, a reduction in vaginal dryness to ease discomfort and pain from sexual intercourse, or as a cure for stress urinary incontinence have expanded rapidly.
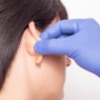
Cosmetic ear surgery or otoplasty can be used to correct ears which stick out, reduce large ears or earlobes, increase the size of small ears, or reshape cartilage in ears with an unnatural shape.

Penis augmentation surgery or penoplasty (penis lengthening and enlargement), is one of the least talked about areas of cosmetic surgery that is available for the male genitalia.

Plasma skin resurfacing (PSR), available from the NeoGen Plasma Skin Regeneration System, uses the energy source of plasma to deliver heat to a targeted treatment area to achieve skin rejuvenation without effecting the surrounding tissues.

Plasma Sublimation or Soft Surgery allows the treatments of the signs of ageing and skin complaints, without actually cutting the skin. It can be used for non-surgical eyelid reconstruction (blepharoplasty), removing lines around the mouth, improvement in the appearance scars and treating a number of skin imperfections.
Learn what polynucleotides are, how they work in the skin, and who they may suit. Clear, evidence-aware guidance for UK patients.
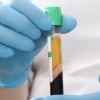
Curious about PRP? Learn what this natural treatment really does for skin, hair, and recovery – without surgery or synthetic fillers.
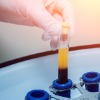
Platelet Rich Plasma (PRP) therapy for sexual rejuvenation. P-shot for men is used to treat erectile dysfunction and to heighten sexual satisfaction. O-shot and Rejuvula for woman is used to reduce vaginal dryness, painful sexual intercourse, and to regain or improve female orgasm.
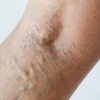
Radiofrequency Ablation or RF Ablation (RFA) is a form of Endovenous Thermal Ablation or Endothermal Ablation (ETA) used to treat varicose veins.
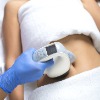
RF energy is able to penetrate deep into the skin causing tissue tightening, heating of fat cells and increased blood circulation for body contouring, fat and cellulite reduction treatments.
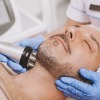
RF energy is able to penetrate deep into the skin and affect the deeper dermis and subcutaneous layers, causing tightening and improvements to the underlying tissue structure for facial rejuvenation.
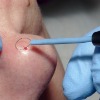
Radiofrequency or radiowave surgery can be used in Dermatology and Cosmetic Medicine for minor surgical procedures such as removing thread veins, warts, growths, birthmarks and moles.
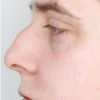
Cosmetic Rhinoplasty or a nose job is a range of surgical procedures which are used to re-shape the nose, or correct nasal deformities to relieve blockages in the nose.
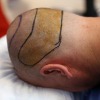
For many years, scalp flap surgery was used by plastic surgeons for the treatment of hair loss after serious scarring had occurred. It has been used for treating male baldness since the early 1980s.
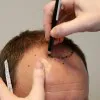
The most common treatment for male baldness is hair transplantation. However, if you have already lost too much hair, scalp reduction surgery can reduce the scalp size to make you look less bald.
Common scars that affect many people include acne and chicken pox scars. Less common raised, red scars known as keloid scars or atrophic scars where the scar tissue is sunken away from the level of the normal skin surrounding it are able to be treated with the application of various products.
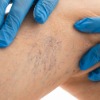
Sclerotherapy was developed for treating varicose veins. Microsclerotherapy is a technique of injecting thread veins with a sclerosant that causes swelling in the vein’s wall which destroys it.

There are many hundreds of different types of cosmeceutical skin care products on the market today that contain active ingredients and claim they can improve wrinkles and the appearance of ageing.
SPF, UVA, UVB? All too confusing? Dermatologists recommend daily use of a broad-spectrum (covering a wide range of wavelengths) UVA and UVB sunscreen with a Sun Protection Factor (SPF) of at least 15.
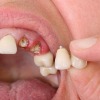
Your dentist can restore teeth to a more natural, pleasing appearance with a variety of different techniques and procedures including replacement fillings, bonding, crowns and bridges.

Tooth bleaching or whitening is not new in dentistry; in fact some techniques are 120 years old! Modern whitening, however, is simple, safe and involves no major dental work or damage to your teeth.
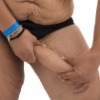
A thigh lift (sometimes known as a thighplasty) is part of a cosmetic surgery procedure called body contouring which is designed to remove large amounts of skin and fat from the hips and thighs.

Thread lift uses free floating cogged (barbed) or smooth sutures for lifting sagging tissue in the face and neck. It is marketed as APTOS Thread Lift, Contour Lift, Silhouette Soft, Scarless Suture Lift & Feather Lift.
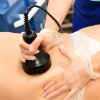
Ultrasonic Body Contouring, available in the UK using the Ultrashape® and LipoSonix® devices, is the latest, minimally invasive way of effectively removing excess fat cells from the abdomen, thighs & flanks.

Ultrasonic skin tightening, introduced with a device called Ultherapy, is a non-invasive, non-surgical cosmetic procedure that uses micro-focused ultrasound waves to stimulate collagen production, resulting in an uplifted effect to the face and neck.
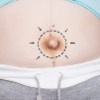
Umbilicoplasty (navel or belly button surgery) is an operation involving making an “outie” belly button into an “innie”, or making an “innie” a little less obvious by lessening the size of the hole.

An upper arm lift or brachioplasty is part of a cosmetic surgery procedure called body contouring which is designed to remove excess saggy skin and fat from the upper arms.