Acne is one of the most common skin conditions, yet the reasons behind it are frequently misunderstood. Breakouts are often blamed on factors such as poor hygiene or individual foods, but acne usually develops through a combination of processes taking place within the skin. Oil production, blocked pores, bacteria, and inflammation interact with hormones and individual skin biology to create the spots that appear on the surface.
Because several factors may be involved at the same time, identifying the causes of acne can feel confusing. Two people with similar-looking breakouts may have very different underlying triggers. For some individuals, hormones or genetics play a stronger role. For others, lifestyle factors, skincare products, or certain medications may contribute to flare-ups. Understanding this complexity is important, as it explains why acne does not respond to a single universal treatment.
This guide explains the main causes of acne in clear terms. It looks at the biological processes that lead to blocked pores and inflammation, how hormones and genetics influence the skin, and the external factors that may aggravate breakouts. It also outlines when persistent acne may benefit from professional assessment within the UK healthcare or aesthetic clinic setting.
To begin, it helps to understand why identifying the underlying causes of acne is an important first step before considering treatment options.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Why Understanding The Cause Of Acne Matters Before Choosing Treatment
Acne is a common skin condition, but the causes of acne breakouts are often misunderstood. Understanding what triggers acne beneath the skin can help guide safer and more effective treatment choices, whether through skincare, medical advice, or professional treatments.
Acne is not caused by dirty skin
A frequent misconception is that acne develops because the skin is not clean enough. In reality, acne forms within the skin’s pores rather than on the surface.
-
Acne begins when hair follicles become blocked with oil and dead skin cells.
-
These changes happen beneath the skin, so surface cleansing alone cannot prevent breakouts.
-
Excessive washing or harsh scrubbing may irritate the skin barrier and increase redness or inflammation.
For most people, gentle cleansing twice daily with a non-comedogenic product is sufficient. Over-cleansing can sometimes make acne-prone skin more reactive rather than clearer.
Acne develops inside the hair follicle
Each pore in the skin contains a hair follicle and a small oil-producing gland called a sebaceous gland. These glands produce sebum, an oily substance that helps protect and moisturise the skin.
Acne begins when several processes occur together:
-
The sebaceous glands produce more oil than the skin needs.
-
Dead skin cells accumulate and block the pore opening.
-
Oil and skin cells form a plug inside the follicle.
-
Naturally occurring skin bacteria can multiply within the blocked pore.
This process leads to the formation of different types of acne lesions, including blackheads, whiteheads, and inflamed spots. Acne most commonly appears in areas where sebaceous glands are more active, such as the face, chest, shoulders, and back.
Understanding how acne develops is important because treatments usually target one or more parts of this process, such as reducing oil production, preventing blocked pores, or calming inflammation.
Acne is rarely caused by a single factor. It develops through a combination of oil production, blocked pores, bacterial growth, and inflammation within the skin.
Excess Oil Production And Blocked Pores
One of the main biological causes of acne breakouts is the combination of excess oil production and blocked pores. These processes occur naturally in the skin, but in acne-prone individuals, they can become more active or less well-regulated.
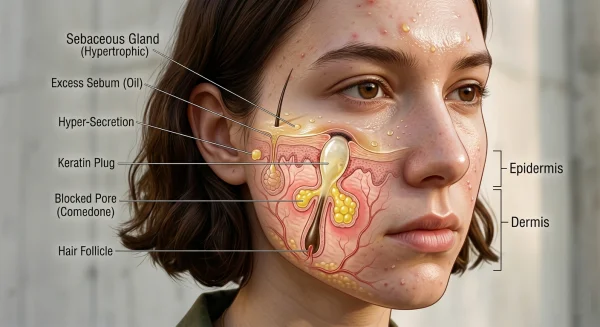
The role of sebum in acne development
Sebum is the oily substance produced by sebaceous glands located alongside hair follicles. It helps keep the skin moisturised and protects the surface barrier.
In acne-prone skin, sebaceous glands may produce more oil than the skin requires.
-
Increased sebum creates a thicker environment inside the pore.
-
This can make it easier for pores to become blocked.
-
Higher oil levels can also support the growth of acne-related bacteria.
Hormones are one of the strongest influences on sebum production. This is why acne often appears during puberty and may fluctuate during hormonal changes in adulthood.
For some people, naturally oily skin increases the likelihood of breakouts, particularly on the forehead, nose, chin, chest, and back.
Dead skin cells and clogged pores
Healthy skin continually renews itself by shedding dead skin cells. Normally, these cells rise to the surface and are removed naturally.
In acne-prone skin, this process can become less efficient.
-
Dead skin cells accumulate inside the pore rather than shedding normally.
-
These cells mix with sebum and create a plug within the follicle.
-
When the pore remains closed, a whitehead may form.
-
When the pore remains open, the plug oxidises and appears as a blackhead.
Blocked pores are known as comedones, which are the earliest stage of acne lesions. Preventing or reducing pore blockage is therefore an important focus of many acne treatments.
Excess oil production and the buildup of dead skin cells can combine to clog pores and trigger the first stage of acne. Once this environment forms within the follicle, other factors, such as bacteria and inflammation, can trigger visible breakouts.
Bacteria And Inflammation In Acne
Once a pore becomes blocked, the environment inside the follicle changes. This is where bacteria and inflammation in acne begin to play a role in turning a blocked pore into a visible breakout.
The role of Cutibacterium acnes bacteria
The skin naturally contains many types of bacteria. One of these is Cutibacterium acnes, a bacterium that normally lives harmlessly on healthy skin.
When a pore becomes blocked with oil and dead skin cells, conditions inside the follicle change.
-
The blocked pore traps oil and reduces oxygen levels.
-
This environment allows Cutibacterium acnes to multiply more easily.
-
As bacteria grow within the follicle, the body’s immune system reacts.
This immune response contributes to redness and swelling around the pore. It is important to note that acne is not contagious. The bacteria involved are part of the normal skin microbiome.
Clinical guidance also emphasises that antibiotics should not be used alone for acne treatment, as combination approaches are usually more effective and reduce the risk of resistance.
Why do some breakouts become inflamed?
Not all blocked pores become inflamed. Some remain as blackheads or whiteheads without redness or discomfort.
Inflammation occurs when the immune system reacts strongly to bacteria and the blocked follicle.
-
The follicle wall may rupture beneath the skin.
-
Inflammatory chemicals are released into the surrounding tissue.
-
This leads to red, swollen spots known as papules or pustules.
-
In deeper cases, nodules or cysts may form.
Inflammatory acne can be more uncomfortable and may carry a higher risk of scarring if left untreated.
The severity of inflammation varies between individuals and is influenced by genetics, hormones, and the body’s immune response.
Bacteria are only one part of the acne process. Breakouts usually develop when blocked pores, excess oil, bacterial growth, and inflammation interact within the skin.
Hormonal Changes And Acne
Hormones are one of the most significant factors influencing acne breakouts. Changes in hormone levels can increase oil production in the skin, which makes blocked pores and inflammation more likely.
Hormonal activity affects people at different stages of life, which is why acne can appear during adolescence and sometimes persist or recur in adulthood.
Puberty and teenage acne
Acne commonly begins during puberty because hormone levels rise rapidly during this stage of development.
-
The hormone testosterone increases in both boys and girls during puberty.
-
Testosterone stimulates the sebaceous glands to produce more sebum.
-
Increased oil production raises the likelihood of blocked pores and acne lesions.
This is why acne often develops on the face, chest, and back during the teenage years. These areas contain a higher concentration of sebaceous glands.
In many individuals, acne improves as hormone levels stabilise in early adulthood. However, this is not always the case.
Hormonal acne in adults
Hormonal changes can also influence acne in adulthood, particularly in women.
Breakouts linked to hormonal fluctuations may appear:
-
before or during menstrual cycles
-
during pregnancy
-
during perimenopause or menopause
-
alongside hormonal conditions such as polycystic ovary syndrome (PCOS)
Adult hormonal acne often appears along the lower face, jawline, and neck, although patterns can vary.
Medical guidance notes that when acne begins suddenly in adult women, particularly alongside symptoms such as irregular periods or increased facial hair, clinicians may assess for underlying hormonal conditions, including PCOS.
Hormonal influences can also affect how persistent or severe acne becomes. For some individuals, breakouts fluctuate with hormonal cycles, while others experience more ongoing acne.
Hormones influence oil production and play a major role in when and where acne develops. However, hormonal changes rarely act alone and often interact with other factors such as genetics, skincare habits, and lifestyle.
Genetic And Biological Factors
While hormones and skin biology influence the development of acne, genetic and biological factors can also affect a person's likelihood of experiencing acne and its severity. These factors help explain why some people develop persistent breakouts while others rarely experience them.
Family history and acne risk
Acne often runs in families. If close relatives experienced acne, particularly moderate or severe acne, the likelihood of developing similar skin patterns may be higher.
-
Genetics can influence the activity of sebaceous glands.
-
Some individuals naturally produce more sebum than others.
-
Genetic traits may also affect how the immune system responds to skin inflammation.
Research suggests that if both parents experienced acne, the risk of developing acne at a younger age or with greater severity may increase.
However, genetics do not guarantee that someone will develop acne. Many people with a family history of acne have only mild symptoms or none at all.
Skin type and sensitivity
Biological differences in skin type can also influence how acne develops.
-
Oily skin tends to produce more sebum, which increases the likelihood of blocked pores.
-
Combination skin may experience breakouts in oilier areas such as the forehead, nose, and chin.
-
Differences in pore size and skin cell turnover can also affect how easily pores become clogged.
The skin barrier also plays an important role. When the barrier becomes irritated or compromised, inflammation may increase, and existing acne can appear more noticeable.
These biological differences explain why acne treatments often need to be personalised. A treatment that works well for one person may not be suitable for another.
Genetics and individual skin biology influence how acne develops and how the skin responds to inflammation. These factors often interact with hormones, skincare products, and lifestyle triggers.
Lifestyle And Environmental Triggers
While the main causes of acne occur within the skin, certain lifestyle and environmental factors can influence how frequently breakouts occur or how severe they become. These triggers rarely cause acne on their own, but they may aggravate underlying acne-prone skin.
Understanding these influences can help people recognise patterns in their breakouts and make informed adjustments to skincare or daily habits.
Stress, sleep, and hormonal fluctuations
Periods of stress can affect several biological processes linked to acne.
-
Stress increases the release of hormones such as cortisol.
-
Higher cortisol levels may stimulate sebaceous glands and increase oil production.
-
Stress can also influence inflammation within the body, which may worsen existing acne.
Sleep patterns may also affect skin health.
-
During sleep, the skin undergoes repair and renewal processes.
-
Ongoing sleep disruption may affect hormone balance and skin barrier function.
-
Poor sleep can make inflammatory skin conditions appear more persistent.
These factors do not directly cause acne, but they may contribute to flare-ups in people who are already prone to breakouts.
Diet and acne research
Diet has been widely discussed in relation to acne, although the scientific evidence remains complex.

Current research suggests that certain dietary patterns may influence acne in some individuals.
-
Diets high in high-glycaemic index (GI) foods may increase insulin levels, which can influence hormone activity and sebum production.
-
Some studies have explored links between dairy intake and acne, although findings remain mixed and not all individuals are affected.
-
A balanced diet that supports overall health is generally recommended.
At present, no single diet has been proven to prevent or cure acne. Individual responses to food can vary, and diet is usually only one part of the wider picture.
Lifestyle factors such as stress, sleep, and diet may influence acne severity, particularly in people who already have skin. However, these triggers usually interact with biological factors rather than acting as the sole cause of breakouts.
Skincare Products And Cosmetic Triggers
Certain skincare or cosmetic products can contribute to acne breakouts in some individuals. While most modern formulations are designed to be skin-friendly, ingredients, product texture, and how products are used can influence whether pores become blocked.
Understanding how products interact with acne-prone skin can help reduce avoidable triggers and support a more suitable skincare routine.
Comedogenic ingredients and pore blockage
Some skincare ingredients are described as comedogenic, meaning they can clog pores in certain skin types.
-
Heavier oils or waxes may sit on the skin surface and contribute to pore blockage in acne-prone individuals.
-
Occlusive products can trap oil and dead skin cells inside the follicle.
-
Products labelled non-comedogenic are generally formulated to reduce the risk of pore blockage.
However, reactions vary between individuals. Another may well tolerate a product that causes breakouts for one person.
For people prone to acne, dermatology guidance often recommends choosing lightweight, oil-free formulations and avoiding overly heavy moisturisers or cosmetic products.
Hair products and friction-related acne
In some cases, acne may be influenced by external factors such as hair products or physical friction.
-
Certain hair styling products can spread onto the skin around the hairline, forehead, or neck.
-
Oils or wax-based formulations may increase the risk of blocked pores in these areas.
-
Friction from clothing, helmets, sports equipment, or bags can irritate hair follicles.
This type of irritation is sometimes referred to as acne mechanica. It is commonly seen in areas exposed to repeated pressure, sweat, or friction.
Recognising these patterns can help identify whether breakouts are linked to external triggers rather than underlying skin conditions.
Skincare and cosmetic products do not cause acne for everyone, but certain formulations or ingredients may contribute to pore blockage in acne-prone skin. Adjusting product choices can sometimes reduce avoidable breakouts.
Medications And Medical Conditions Linked To Acne
In some cases, acne breakouts may be influenced by medications or underlying health conditions. These factors can affect hormone levels, oil production, or skin inflammation, which may increase the likelihood of acne developing or worsening.
Identifying these influences can be helpful when acne appears suddenly, changes pattern, or does not respond to typical treatments.
Medications that may trigger acne
Certain medicines are known to contribute to acne in some individuals. This does not mean everyone taking these medications will develop acne, but they may increase the risk of breakouts.
Examples include:
-
Steroid medications, including oral or topical corticosteroids.
-
Lithium is sometimes used in the management of certain mental health conditions.
-
Some antiepileptic medications.
-
Certain hormonal medications.
These medicines can influence inflammation, hormone balance, or oil production within the skin.
If acne begins soon after starting a new medication, it may be helpful to discuss this with a healthcare professional. Adjustments to treatment should only be made with medical guidance.
Hormonal conditions affecting acne
Some medical conditions can influence hormone levels and may contribute to acne.

One example is polycystic ovary syndrome (PCOS), a hormonal condition that can affect women.
Symptoms that may appear alongside acne include:
-
irregular menstrual cycles
-
increased facial or body hair
-
thinning hair on the scalp
-
persistent acne affecting the lower face
Healthcare professionals may investigate these symptoms using blood tests or ultrasound imaging when appropriate.
When acne is linked to hormonal imbalance, treatment may involve addressing the underlying condition alongside managing the skin symptoms.
Medications and certain medical conditions can influence acne by affecting hormones, inflammation, or oil production. Recognising these factors can help ensure acne is assessed and managed appropriately.
Why Acne Causes Differ Between Individuals
Acne develops through a combination of biological processes, but the causes of acne breakouts can vary significantly between individuals. Two people may experience similar-looking spots, yet the underlying triggers may be different.
This variation explains why acne treatments are often personalised rather than relying on a single universal approach.
Multiple factors often interact.
Acne rarely develops from a single cause. Instead, several factors usually interact within the skin.
These may include:
-
increased oil production from sebaceous glands
-
accumulation of dead skin cells blocking pores
-
growth of naturally occurring skin bacteria
-
inflammation within the follicle
-
hormonal fluctuations
-
external triggers such as skincare products or friction
When several of these processes occur together, the likelihood of breakouts increases.
For example, someone with naturally oily skin may experience acne primarily due to excess sebum and blocked pores. Another person may develop acne mainly during hormonal fluctuations or stress-related changes.
Recognising that acne is multifactorial helps explain why treatment often targets more than one mechanism within the skin.
Why acne may persist without treatment
Acne can sometimes resolve on its own, particularly in adolescence. However, in many cases, the underlying processes continue unless they are managed.
Without treatment:
-
blocked pores may continue forming new spots
-
Inflammation can become more persistent
-
deeper lesions may develop in some individuals
-
Post-inflammatory marks or scarring may occur
Clinical guidance also highlights that untreated moderate or severe acne can lead to longer-term skin changes and may benefit from earlier medical assessment.
Because acne develops through several overlapping mechanisms, treatment plans often combine different approaches. These may include topical treatments, medical therapies, or professional skin treatments, depending on the severity and cause.
Acne does not develop the same way for everyone. Differences in hormones, skin biology, genetics, and lifestyle factors mean that each person’s acne pattern may have its own combination of triggers.
When To Seek Professional Advice For Acne
Many people experience occasional breakouts that can be managed with appropriate skincare or over-the-counter treatments. However, acne breakouts sometimes require professional advice, particularly when symptoms persist or become more severe.

Early assessment can help identify the underlying causes of acne and guide appropriate treatment options.
Signs that acne may require medical assessment
Some types of acne may benefit from medical or dermatological evaluation.
Situations where professional advice may be appropriate include:
-
Moderate to severe acne, particularly with widespread inflamed spots.
-
Painful nodules or cysts that develop deep beneath the skin.
-
Acne that persists despite consistent use of over-the-counter treatments.
-
Breakouts that lead to visible scarring or persistent pigmentation changes.
-
Acne that significantly affects confidence or psychological well-being.
Clinical guidance notes that acne severity is often categorised by the types of lesions present. Mild acne usually involves blackheads and whiteheads, while more severe forms may include painful nodules or cysts.
When acne becomes persistent or severe, early treatment can help reduce the risk of long-term skin changes.
Treatment pathways available in the UK
Several treatment pathways are available depending on the severity and underlying cause of acne.
Common options include:
Over-the-counter treatments
-
Products containing ingredients such as benzoyl peroxide or azelaic acid.
-
Suitable for many cases of mild acne.
GP-prescribed treatments
-
Topical retinoids or combination topical therapies.
-
Oral antibiotics are used alongside topical treatments in moderate acne.
-
Hormonal treatments in selected cases.
Dermatology referral
-
For acne that does not improve after standard treatments.
-
Dermatologists may consider medications such as isotretinoin for severe acne.
Professional clinic treatments
Some aesthetic clinics provide non-surgical treatments that may support acne management or help improve the appearance of acne-prone skin.
These may include:
-
chemical peels
-
light-based treatments
-
ultrasound-based technologies such as LDM Triple
-
microneedling for acne-related skin concerns
Professional consultation is important for assessing suitability and ensuring treatments are used appropriately alongside medical care when needed.
Acne can vary widely in severity and underlying causes. When breakouts are persistent, painful, or affecting confidence, professional advice can help guide safe and effective treatment options.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.


