Hormonal acne in women is a common but often misunderstood topic. Many people assume acne is mainly a teenage issue or that adult breakouts are caused by the wrong skincare, stress, or poor routine. In practice, hormonal acne is usually more complex than that. It can be influenced by menstrual cycles, perimenopause, pregnancy, polycystic ovary syndrome, and individual sensitivity to hormones, even when hormone levels are not obviously abnormal.
That complexity is one reason the subject can feel difficult to navigate. Advice is often inconsistent, treatment timelines are not always clear, and there is a lot of confusion around what counts as hormonal acne compared with other forms of adult acne. For anyone trying to make informed decisions, whether about products, medical treatment, or professional support, it helps to start with a straightforward explanation of what is known, what varies, and what usually matters most in practice.
This guide sets out the basics in a structured way. It explains what hormonal acne is, what may cause it, how it is diagnosed, and which treatment options are commonly considered in the UK. It also covers realistic treatment timelines, possible side effects, the emotional impact of persistent acne, and how to think through the most suitable next step for your circumstances.
The most useful place to begin is with what hormonal acne in women is, and how it differs from other common acne patterns.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
What Is Hormonal Acne In Women, And How Is It Different?
Hormonal acne in women refers to breakouts influenced by internal hormone fluctuations rather than surface-level triggers alone. It often appears in adulthood and follows recognisable patterns that differ from teenage acne.
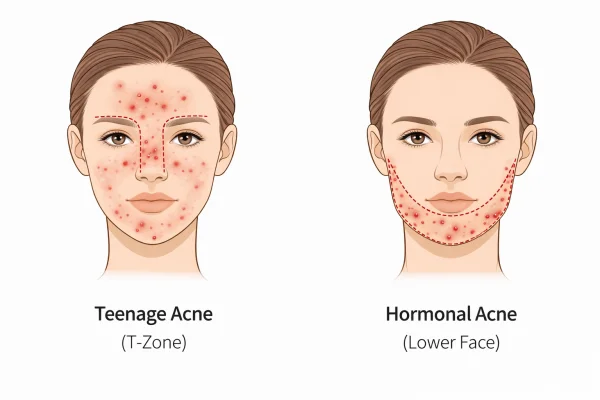
What defines hormonal acne
-
Hormonal acne is linked to sensitivity to androgens, hormones that increase oil (sebum) production in the skin.
-
This excess oil combines with dead skin cells, leading to blocked pores and inflammation.
-
It is not caused by poor hygiene, and over-cleansing can worsen symptoms.
How hormonal acne presents on the skin
-
Commonly appears along the jawline, chin, and lower cheeks.
-
Lesions tend to be deeper, inflamed, and sometimes painful, rather than small surface spots.
-
Breakouts often follow a cycle, for example, worsening before a menstrual period.
How it differs from other types of acne
-
Teenage acne often affects the forehead and T-zone, whereas hormonal acne is more concentrated on the lower face.
-
Adult hormonal acne may be persistent or recurring, even with a consistent skincare routine.
-
It is more likely to be influenced by internal factors, such as hormonal changes, rather than external triggers alone.
Why does it often develop in adulthood
-
Hormone fluctuations linked to the menstrual cycle, pregnancy, or perimenopause can trigger breakouts.
-
Some women develop acne for the first time in their late twenties or beyond.
-
Conditions such as polycystic ovary syndrome (PCOS) may also contribute in certain cases.
Hormonal acne can feel confusing, particularly when it appears later in life or does not respond to typical skincare approaches. Recognising its pattern is the first step towards choosing treatment options that address the underlying cause, not just the visible symptoms.
Hormonal acne is defined by where it appears, how it behaves, and what drives it beneath the surface. Understanding these differences helps guide more appropriate and effective treatment choices.
What Causes Hormonal Acne In Women?
Hormonal acne in women develops through a combination of internal hormonal activity and changes within the skin itself. Understanding these causes helps explain why breakouts can feel persistent and difficult to manage with skincare alone.
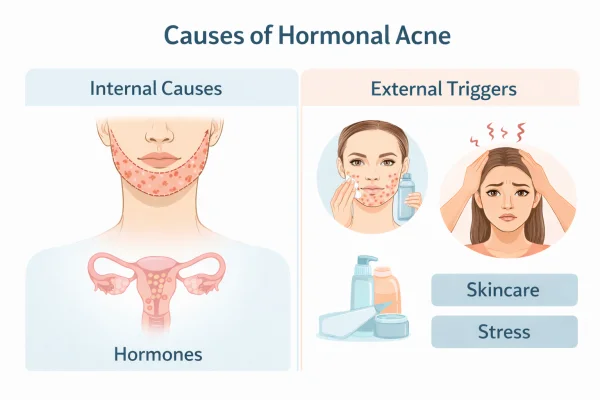
The role of hormones and androgens
-
Hormonal acne is driven by androgens, including testosterone, which increase oil production in the skin.
-
Higher sebum levels can mix with dead skin cells, leading to blocked pores and inflammation.
-
In many cases, hormone levels are within a normal range, but the skin is more sensitive to these changes.
Common hormonal triggers in adult women
-
Menstrual cycle: Breakouts often appear in the days leading up to a period due to hormonal shifts.
-
Pregnancy and post-pregnancy changes: Fluctuating hormone levels can trigger new or worsening acne.
-
Perimenopause and menopause: Hormonal instability during this stage can lead to adult-onset acne.
-
Polycystic ovary syndrome (PCOS): A hormonal condition that may present with acne alongside other symptoms such as irregular periods.
Additional contributing factors
-
Genetics: A family history of acne can increase the likelihood and severity.
-
Stress: Elevated cortisol levels may influence oil production and inflammation.
-
Skincare and cosmetics: Products that block pores can worsen existing acne.
-
Lifestyle factors: Smoking and high glycaemic diets may contribute in some individuals.
These factors often work together rather than in isolation, which is why hormonal acne can vary significantly between individuals.
Why it can feel unpredictable
-
Hormonal fluctuations do not follow a fixed pattern for everyone.
-
External factors such as stress or changes in skincare can amplify underlying hormonal activity.
-
This combination can lead to cycles of improvement and flare-ups, even when routines remain consistent.
Hormonal acne is not caused by a single factor but by an interaction between hormones, skin biology, and individual triggers. Recognising these layers makes it easier to approach treatment in a structured and realistic way.
How Is Hormonal Acne Diagnosed?
Hormonal acne in women is usually diagnosed through a clinical assessment rather than tests. The process focuses on recognising patterns, understanding your history, and assessing how the skin is behaving over time.
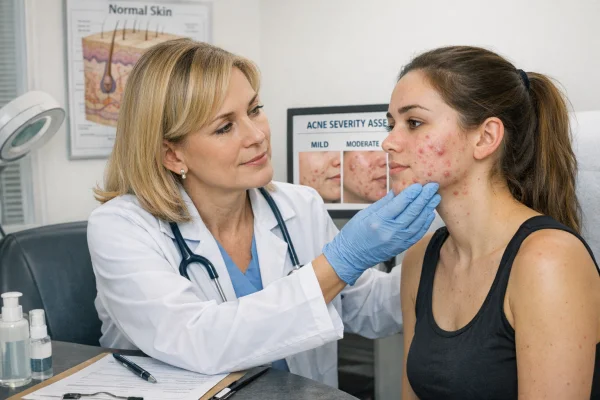
Clinical assessment and pattern recognition
-
A GP, dermatologist, or experienced practitioner will examine the skin and identify the types of spots present, such as inflamed lesions or deeper nodules.
-
The location of breakouts is an important clue, with hormonal acne commonly affecting the jawline, chin, and lower face.
-
The clinician will assess severity, typically categorised as mild, moderate, or severe, which helps guide treatment decisions.
-
Diagnosis is usually made visually, as acne has a recognisable appearance and distribution.
Questions you are likely to be asked
-
When did the acne start, and has it changed over time?
-
Does it follow a cyclical pattern, for example, around your menstrual cycle?
-
What treatments or skincare have you already tried?
-
Are there any other symptoms, such as irregular periods or excess hair growth?
These questions help build a clearer picture of whether hormones are playing a significant role.
When further investigation may be needed
-
If acne develops suddenly in adulthood or persists and is resistant to treatment.
-
If there are signs of an underlying hormonal condition, such as PCOS.
-
In these cases, a GP may recommend blood tests or referral to a specialist for further assessment.
Why is diagnosis often straightforward
-
Acne is a common condition with well-established clinical patterns.
-
Most cases do not require scans or complex investigations.
-
The focus is on identifying the type and cause so that treatment can be matched appropriately.
Diagnosing hormonal acne is usually a clear and structured process based on visible signs and personal history. The value lies in understanding what is driving your acne, so the next steps are targeted and appropriate.
Treatment Options For Hormonal Acne In The UK
Hormonal acne in women is usually managed through a combination of skincare, medical treatment, and, in some cases, clinic-based therapies. The approach is stepwise, meaning treatment is adjusted based on severity, response, and individual factors.
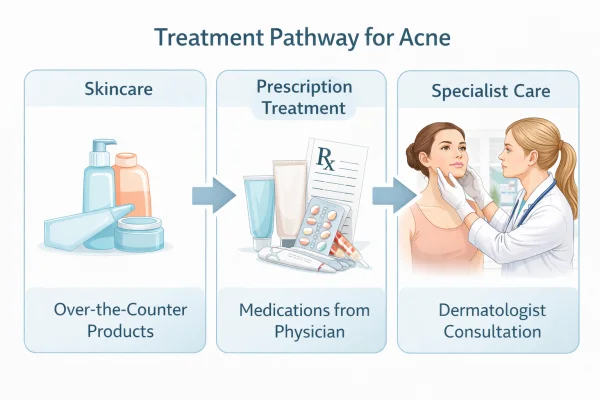
Over-the-counter and skincare approaches
-
Start with non-comedogenic cleansers and moisturisers to avoid blocking pores.
-
Active ingredients such as benzoyl peroxide, azelaic acid, and niacinamide can help reduce inflammation and prevent new breakouts.
-
Products should be used consistently across the affected area, not just on individual spots.
-
Improvements are gradual, often taking several weeks before visible change.
This stage is typically suitable for mild acne or as part of a broader treatment plan.
Prescription treatments
-
Topical retinoids help regulate skin cell turnover and prevent blocked pores.
-
Combination treatments (for example, retinoid with benzoyl peroxide or antibiotics) are commonly recommended.
-
Oral antibiotics may be used for moderate acne but are time-limited to reduce resistance.
-
Hormonal treatments, such as spironolactone, may be considered in adult women with persistent acne.
-
Isotretinoin is reserved for severe or treatment-resistant acne and requires specialist supervision.
Treatment is usually reviewed at around 12 weeks to assess progress and adjust if needed.
Professional and clinic-based treatments
-
Chemical peels can help improve skin texture and reduce congestion.
-
Light-based therapies may support reduction in inflammation and bacteria.
-
Ultrasound-based treatments, including LDM Triple, are sometimes used to support skin healing and barrier function.
-
These treatments are typically used alongside medical or topical therapies, rather than as standalone solutions.
A consultation is important to determine suitability, particularly for persistent or hormonally driven acne.
Why combination treatment is often needed
-
Hormonal acne involves multiple factors, including oil production, inflammation, and pore blockage.
-
Addressing only one aspect may lead to limited or temporary improvement.
-
A combined approach allows treatment to be adjusted over time, depending on response.
Treatment for hormonal acne in the UK follows a structured pathway, starting with simple measures and progressing when needed. The most effective plans are tailored, combining medical guidance with consistent skincare.
Acne Treatment Pathway
Hormonal acne treatment takes time, and progress is usually gradual rather than immediate. Understanding realistic timelines can help you stay consistent and avoid changing treatments too quickly.
Early stages and adjustment period
-
In the first few weeks, some treatments can cause dryness, irritation, or mild worsening of breakouts.
-
This is often linked to ingredients such as retinoids increasing skin cell turnover.
-
Starting slowly, for example using products on alternate days, can help improve tolerance.
-
It is generally recommended to continue treatment unless side effects are severe.
Medium-term improvement
-
Noticeable improvement often begins around 6 to 8 weeks, with fewer inflamed spots and reduced oiliness.
-
Skin may start to feel more balanced, although breakouts can still occur intermittently.
-
Consistency is important, as stopping and restarting treatment can delay progress.
Review and adjustment at 12 weeks
-
Treatment is typically reviewed at around 12 weeks to assess response and side effects.
-
If improvement is limited, treatment may be adjusted or escalated.
-
If acne has improved, maintenance strategies are usually introduced to prevent relapse.
Long-term management
-
Hormonal acne often requires ongoing management, even after improvement.
-
Maintenance may include continued topical treatments or periodic review.
-
Relapses can occur, particularly during hormonal changes, but are usually manageable with early intervention.
Hormonal acne treatment is a process that unfolds over weeks and months, not days. Setting realistic expectations supports better adherence and more stable long-term results.
Risks, Side Effects, And Limitations
Hormonal acne treatments are generally safe when used appropriately, but they do carry potential side effects and limitations. Understanding these in advance helps you make balanced decisions and avoid unnecessary concern if mild reactions occur.
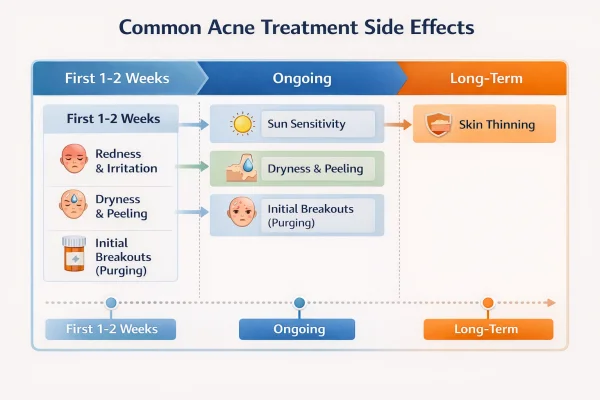
Common side effects of topical treatments
-
Dryness, redness, and irritation are common, particularly in the early stages.
-
Ingredients such as retinoids and benzoyl peroxide can increase skin sensitivity, including to sunlight.
-
Gradual introduction, for example, starting a few times per week, can improve tolerance.
These effects are usually temporary and settle as the skin adjusts.
Considerations with oral and hormonal treatments
-
Oral antibiotics are typically used for limited periods to reduce the risk of resistance.
-
Hormonal treatments, such as spironolactone, may not be suitable for everyone and require medical assessment.
-
Isotretinoin is highly effective for severe acne but requires close monitoring due to potential side effects and strict prescribing guidelines.
Decisions around these treatments are made on an individual basis, taking into account medical history and treatment response.
Limitations of treatment
-
There is no immediate or permanent cure for acne, and results take time.
-
Responses vary, meaning a treatment that works well for one person may be less effective for another.
-
Hormonal fluctuations can continue to trigger breakouts, even with treatment in place.
A structured, adaptable plan is often more effective than relying on a single product or approach.
Risks of delaying or avoiding treatment
-
Persistent inflammation can increase the likelihood of scarring or pigmentation changes.
-
Repeated cycles of untreated acne may make the condition harder to control over time.
-
Early, appropriate treatment can reduce these longer-term effects.
Most hormonal acne treatments are well established and safe under guidance, but they require realistic expectations and ongoing review. Understanding both benefits and limitations supports more confident, informed decisions.
Choosing The Right Treatment Approach For You
Selecting the right approach to hormonal acne in women depends on more than the type of spots alone. It involves understanding your skin and health, and determining the appropriate level of treatment at each stage.

Factors that influence treatment decisions
-
Severity and type of acne: Mild, moderate, and severe acne require different levels of intervention.
-
Pattern and triggers: Cyclical breakouts or hormonal patterns may guide treatment choice.
-
Medical history: Existing conditions, medications, and suitability for hormonal treatments are considered.
-
Skin sensitivity: Some treatments may need to be introduced gradually to reduce irritation.
-
Lifestyle factors: Time, routine, and consistency can affect the practicality of certain treatments.
A tailored plan is usually more effective than a standardised approach.
Questions to ask during a consultation
-
What type of acne do I have, and is it hormonally driven?
-
What treatment options are suitable for my level of severity?
-
How long is it likely to take before I see improvement?
-
What side effects should I expect, and how can they be managed?
-
What happens if the treatment does not work as expected?
These questions help ensure expectations are realistic and decisions are informed.
NHS vs private treatment pathways
-
NHS care: Typically starts with GP-led treatment, with referral to dermatology for more severe or resistant cases.
-
Private clinics: May offer quicker access to consultations and a wider range of treatment options, including clinic-based therapies.
-
Both pathways follow similar clinical principles, but access, timelines, and available treatments can differ.
Choosing between them often depends on urgency, preference, and access rather than quality of care alone.
The importance of ongoing review
-
Acne treatment is rarely static and often requires adjustment over time.
-
Regular review helps assess progress, manage side effects, and refine the plan.
-
Early changes can prevent unnecessary delays in finding an effective approach.
The most effective treatment approach for hormonal acne is one that reflects your individual pattern, severity, and preferences. Clear guidance and regular review support better outcomes over time.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.


