Procedure Time: Approx. 30 minutes
Recovery Time: Walk-in walk-out procedure. Soreness for a few days.
Results Duration: Longer lasting than traditional surgical stripping.
Cost: Private prices range from £2,000 to £5,000.
Anaesthesia: Ultrasound is used to guide local anaesthetic injections to surround the vein with tumescent local anaesthetic.
For a full list of FAQs please Click Here.
For confirmed cases of varicose veins, NICE recommends that endothermal ablation, radiofrequency or laser, should be offered. If endothermal treatment is not suitable, then ultrasound-guided foam sclerotherapy should be offered. Endovenous Thermal Ablation or Endothermal Ablation (ETA) describes certain treatments used for targeting refluxing superficial veins which use heat energy delivered from inside the vein under local anaesthesia, as a treatment for varicose veins. When laser is used as the energy source it is called Endovenous Laser Ablation (EVLA), but Radiofrequency can also be used in a treatment called Radiofrequency Ablation or RF Ablation (RFA). RFA is a process of heating a vein sufficiently so that the tissue contracts tightly during the heating process, closing the vein, and the cells in the vein wall die so that the vein can never reopen again. The cost of RFA will depend on the number of varicose veins being treated, the severity of them and whether one leg or both legs is being treated. Private prices range from £2,000 to £5,000.
We would like to thank Vascular Surgeon Prof Mark Whiteley from The Whiteley Clinic for his expert medical help.
Endovenous Thermal Ablation or Endothermal Ablation (ETA) is the generic term for all methods of treating refluxing superficial veins using heat energy delivered from inside the vein under local anaesthesia. ETA is now the NICE recommended way of treating varicose veins and should have completely replaced stripping.
When laser is used as the energy source the treatment is called Endovenous Laser Ablation (EVLA). Radiofrequency may also be used as a form of ETA for Radiofrequency Ablation or RF Ablation (RFA).
According to a study by CJ Evans et al in 1999, varicose veins are present in approximately 1 in 3 adults in the Western world.
Treatment of varicose veins is generally considered to be a medical matter, although the main implications are usually cosmetic, in that people don’t like to live with the appearance of them, usually on their legs. Pain and discomfort are also a factor. Sufferers are often referred by their GP to a vascular or vein specialist for diagnosis of the problem and to discuss treatment options.
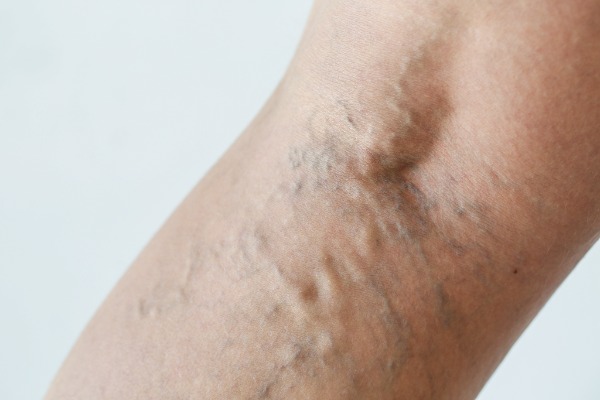
Unlike thread or spider veins, varicose veins are situated beneath the skin, being skin coloured or bluish-green and more than 2mm in diameter. They are more serious than thread veins and they can be painful (or achy) and are a sign of leg pump or venous failure, almost always superficial venous reflux.
Different treatment options are available for varicose veins. Traditional treatment is ligation or tying of the affected veins and stripping them from the leg. This a surgical procedure which requires general anaesthetic and up to six weeks ‘down time’ away from work. As well as being painful, this also leads to the veins growing back again in the majority of cases, a process known as neovascularisation. Although still available on the NHS, this is considered by many vascular specialists to be an outdated and unnecessary form of treatment. Other options include foam sclerotherapy where a sclerosant substance is injected in the vein causing the vein walls to collapse.
In 1999, Consultant Vascular Surgeon, Prof. Mark Whiteley became the first person in the UK to perform ETA using radiofrequency energy – Radiofrequency Ablation (RFA) - to generate the heat inside a vein, thus destroying it and allowing it to be reabsorbed by the body without any regrowth. The procedure was performed using ultrasound guidance, via a tiny keyhole incision of 2 or 3mm.
If you are considering Radiofrequency Ablation for varicose veins, the following information will give you a basic understanding of the procedure. It can't answer all your questions, since a lot depends on your individual diagnosis. Please ask your vascular specialist about anything you don't understand.
Radiofrequency ablation is a process of heating a vein sufficiently so that the tissue contracts tightly during the heating process, closing the vein, and the cells in the vein wall die so that the vein can never reopen again.
It is a catheter based treatment, which means that a very long, thin, tube is passed up inside the vein itself under ultrasound control. This long thin device is called a catheter. It is usually introduced into the vein through a single needle hole just below the knee. Sometimes, depending on anatomy, this site might vary. Because ultrasound scanning is now so good, provided there is a second person performing the ultrasound during the procedure, the top of the catheter can be placed precisely at the point where the target vein meets the deep system.
As heat is going to be generated, it is important to put local anaesthetic around the vein. This is also guided by ultrasound. Local anaesthetic is injected around the vein in very large volumes, not only numbing the vein but also preventing any heat that is generated from affecting any surrounding tissue. This is called tumescence and it causes the vein to contract tightly onto the radiofrequency catheter. The patient is also tipped head down whilst lying on a couch to empty any residual blood from the vein to ensure very good contact between the radiofrequency catheter and the vein wall.
When treatment is to start, the radiofrequency current is turned on. An electric current passes down the catheter into the electrodes positioned at the tip of the device. This allows an electric current to start passing into the vein wall. This current then switches direction, flowing the opposite way. Almost instantly, it switches once again and so on, changing direction thousands of times a second. This frequency of changed direction of current makes all of the electrons in the vein wall vibrate, generating heat. Because the frequency is thousands of times a second, and because radios work when current changes thousands of times a second, the electrical current is said to be operating at radiofrequency rates. Hence the term radiofrequency ablation.
This vibration of the electrons in the vein wall generates sufficient heat to cause the proteins in the vein wall to contract, closing the vein and to kill the cells in the vein wall, making sure the vein cannot grow back again.
As with all good vein surgery, and has now recommended by the National Institute of Health and Clinical Excellence (NICE) in their clinical guidelines CG168, all patients with varicose veins and any symptoms or signs should be assessed by a team of experts. There should be a doctor who examines the patient and decides if it is a vein problem. If it is, then the patient should undergo venous duplex ultrasonography by a specialist (usually a vascular technologist) who specialises in venous duplex ultrasound. Many "cut-price" vein services still exist where doctors do their own duplex ultrasound. Not only are these breaking the NICE guidelines, but research presented in New York several years ago shows that when doctors do their own scans, they miss at least 30% of the problem veins.
Once the specialist vascular technologist has performed a venous duplex, usually taking about 20 minutes per leg, the doctor will see the patient again along with the scans. If the deep veins are working normally, and the varicose veins are actually due to reflux (valves not working) in the truncal veins or perforating veins, radiofrequency ablation or endovenous laser ablation will be recommended for the truncal veins and TRLOP for the treatment of the incompetent perforating veins.
Any surface veins will need to be treated either by removal (phlebectomy) if very large or by injection of sclerotherapy (foam sclerotherapy or liquid sclerotherapy) if smaller.
A medical history will be taken to make sure that there are no reasons why you are not suited to be treated with RFA. Then you would normally be asked to sign a consent form, which means that you have understood what the treatment may do, and the potential side effects.
Photographs may also be taken by the practitioner that can be used as a “before and after” comparison to show you how successful your treatment has been from a cosmetic perspective.
Since 2005, endovenous thermoablation in modern vein clinics and vein practices has been performed under local anaesthetic only, with no general anaesthetic or sedation. In America, this is called "ambulatory surgery" as you literally walk-in and walk-out.
The patient who has already been consented and understands what is going to happen, gets undressed and is taken into the operating theatre. An ultrasound is performed to mark the veins that are going to be treated with radiofrequency ablation as well as any surface veins that might be removed with phlebectomy at the same operation.
The skin of the leg is prepared and sterilised using a special disinfectant fluid, and the patient is covered with surgical drapes to keep the surrounding area sterile.
The bed is tipped head up, to fill the vein with blood. Using an ultrasound probe covered with a sterile cover, the vein is identified. Local anaesthesia is injected under the skin and a needle is passed into the vein. Once the needle is in the vein, a wire can be passed down the needle, a larger catheter can then be passed over the wire and through this and the radiofrequency catheter can be introduced into the vein. This is then passed up the vein to the top, usually in the groin or in the small saphenous vein, in the back of the knee. The ultrasound is used to position the catheter precisely.
The patient is then tipped head down to empty the vein completely. Ultrasound is used to guide local anaesthetic injections to surround the vein with tumescent local anaesthetic.
Once this has been completed the radiofrequency is turned on. Depending on the machine, the vein might then be closed in steps (segments) or might be closed with a constant pullback of the device at a set rate.
In the best practices where a surgeon works with a vascular technologist, the vascular technologist continues to scan the vein during treatment to ensure that the vein is closing adequately. This means that if for any reason the vein does not close, further treatment can be performed immediately.
Once the vein has been closed, any further veins that need treatment can be close the same way. TRLOP will be performed on any incompetent perforators using a very similar technique but, as perforating veins are very small, this is much quicker.
Finally, any bulging surface veins are removed under local anaesthetic using very small holes and hooks. No stitches need to be used at all as all of the incisions are so small nowadays.
Little clasps are placed on all of the wounds, a light bandage placed around the leg to catch any local anaesthetic that may go through the wounds and patients are usually discharged with a stocking covering the bandage.
This is a walk-in walk-out procedure. The area may be a little sore for a few days but it is rare for patients to have any real pain. Some people are very sensitive, particularly if they are thin framed, and might feel more discomfort.
In an audit performed by the Whiteley Clinic, only 1 in 10 need any painkillers. Whether someone feels pain or not, it is sensible to remember that the alternative, stripping, is approximately 10 times more painful and usually stops proper walking or driving for up to 14 days after treatment.
Most people are back to normal walking the same day, driving the following day and get back to normal life including baths and showers between two and five days after the surgery when the little wounds have healed. Depending on the extent of the veins, most people are able to return to sport and the gym between one and three weeks after treatment. It is very rare to have any recovery taking longer than this.
However, it must be remembered that veins have been destroyed, and as such the area might still be tender when pressed up to 3 to 6 months later.
Research has shown that the risks of complications and hence poor quality-of-life is lower than if the veins are not treated at all. This is why vascular surgeons perform the surgery. However, as with all medical interventions, there are possible risks.
Everyone will get some pain and bruising because it is a surgical procedure, but it is important to remember it is so much less painful than stripping. Everyone will get small scars, but compared to the old stripping procedure, these are negligible and in good hands, are rarely visible six months later.
It is possible to get wound infection, deep vein thrombosis or pulmonary embolism although all of these risks are very small. Provided the procedure is done under local anaesthetic, you will be fully mobile and deep vein thrombosis is very unlikely. If general anaesthetic or sedation is used, the risk of deep vein thrombosis increases because the patient mobility decreases and people are often asked not to drink before the procedure. Hence, only local anaesthetic should be used for endovenous surgery.
It is possible to get some numbness after the surgery and this is usually transient. Under local anaesthetic, people can say "ow" and so it is rare to get a permanent nerve damage. Surgeons that still use general anaesthetic or sedation are more likely to causes problem as patients cannot let them know if a nerve is being damaged. This is another reason why true vein experts have not use general anaesthetic or sedation for years.
The area of the vein being treated, usually the inner thigh, can be tender to the touch for a couple of weeks especially if the patient is slim. If the small saphenous vein is treated, then it is the calf that can be tender.
If the radiofrequency has been performed correctly, then the vein should be permanently destroyed and should not come back again. However, in some practices, there can be some technical failures which means that in a small number of patients, the same vein may reopen in the future and need treatment again.
Very rarely, a brown stain might become visible over the area where the vein is treated, or a patch of thread veins may appear. This is often a technical failure where the vein was too close to the skin and should have been treated by a different method. However, it is possible that this can occur in slim patients even when the appropriate techniques are performed.
It is possible to get other varicose veins recurring again from other veins that have not been treated that were normal on the day of treatment.
It is important to follow the advice of your vein specialist as closely as possible following RFA to ensure that you get the full benefit of the treatment and avoid any complications.
Post-treatment advice may include:
· If you have any discomfort, you can take over the counter anti-inflammatories or pain killers (ibuprofen or paracetamol) for a few days after the treatment, which will ensure you feel comfortable.
· Wear the supplied or recommended compression stockings for the time period advised.
· Plan for an average of three days off work post treatment although some people do return to work sooner (even on the same day), this depends on how you feel and your type of work.
· Do plenty of walking post-treatment (ideally four miles per day for two weeks).
· Avoid hot baths, Jacuzzis, steam rooms or swimming pools until the little wounds have healed and you do not have any tenderness.
You should not undergo RFA treatment if you are pregnant and many specialists will not treat patients who are breast feeding.
If there is a history of past deep vein thrombosis (DVT), the ultrasound scan will need to pay particular attention to the state of the deep veins. If there is significant deep vein obstruction, RFA may be inadvisable.
Other contra-indications include:
· If you have had any previous varicose vein surgery, or phlebitis, then you may not be suitable for radiofrequency ablation and may require another endovenous techniques such as endovenous laser ablation.
· If you are on anticoagulation, you can still undergo radiofrequency ablation but you must tell the doctor as it might modify the technique particularly as to whether phlebectomies are performed.
RFA should be performed by a qualified vascular surgeon or interventional radiologist, who is trained and experienced in the delivery of the procedure.
Find a Clinic specialising in Radiofrequency Ablation in the UK & Ireland.
Until recently it was highly unlikely that anyone considering Radiofrequency Ablation for the treatment of varicose veins would’ve been able to access this free of charge on the National Health Service, as the treatment of choice recommend within the health system was vein stripping.
However, the National Institute for Health and Care Excellence (NICE) issued updated guidance at the end of July 2013 which stated that surgery should only be offered to treat varicose veins on the NHS if other less invasive treatments are unsuitable.
Currently there is wide regional variation in the treatment of varicose veins in the UK as there is no definitive system for determining which people would benefit most from treatment. There is also currently no established framework within the NHS for the diagnosis and management of the condition. To help standardise the kind of treatment people can receive, NICE has published a new clinical guideline on varicose veins.
For confirmed cases of varicose veins, it recommends that endothermal ablation, radiofrequency or laser, should be offered. If endothermal treatment is not suitable, then ultrasound-guided foam sclerotherapy should be offered. Finally, if these others are not suitable, then surgery should be considered. The guidance in PDF format is available here.
We would therefore always recommend that you visit your General Practitioner before embarking on private treatment for varicose veins. As well as their advice and guidance they may also be able to refer you to a local NHS Hospital who can treat you with newer techniques, based on this updated guidance.
Please note that results of surgery vary enormously, depending upon the patient, their condition and the skill of the individual surgeon.
We currently do not have any before and after images for radiofrequency treatment for varicose vein procedures.