20
Jun
2013
Acne affects 80% of people at some point in their lives and is the commonest skin condition that people consult their doctor about.
About 20% of acne sufferers will have acne so severe that they will require aggressive medical treatment to avoid the risk of secondary scarring. Acne can have profound and devastating psychosocial consequences and needs to be treated quickly and effectively.
Although the diagnosis of acne is straightforward and effective treatments are available, acne is still a challenging dermatological problem.
There are several reasons for this. Firstly, people commonly delay consulting their doctor for acne in the hope that it will just go away. In adolescents, the average time between the onset of acne and seeking medical help is about 1 year, despite the significant impact it has on self-esteem and psychological well-being.
The second reason is that acne is a chronic skin condition with no quick fixes or overnight cures. Treatments often take 6 to 8 weeks (or longer) to be effective with the result that many people give up on their treatments thinking that they haven’t worked. This results in suboptimal or under-treatment and is another reason why acne presents such a challenge.
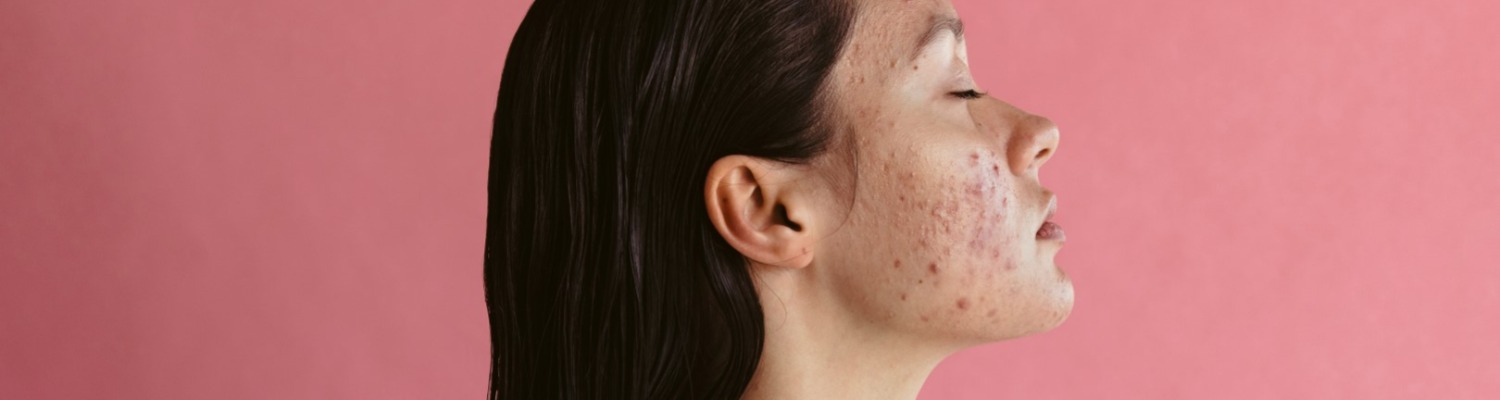
Acne is caused by changes in hormone levels at significant points in our lives. Puberty is the most common time to develop acne and it is caused by an increase in testosterone, regardless of sex. This testosterone surge affects the pilosebaceous unit triggering increased sebum production. Sebum is the body’s natural oil that acts to lubricate the skin and helps maintain the integrity of the skin barrier.
Areas most densely populated by sebaceous glands are the face, chest and upper back hence acne typically affects these areas.
Increases in sebum and keratin in the pilosebaceous unit cause a hyperkeratotic plug to form called a microcomedone.

Microcomedones are the earliest acne lesion and are basically blockages in the follicle. In these conditions the naturally occurring (but largely commensal) organism Propionibacterium acnes uses sebum for growth and then proliferates. In a sebum rich blocked follicle P. acnes contaminates the follicle and causes significant localized inflammation.
Part of the difficulty in treating acne stems from the significant side effects that many traditional medical treatments cause. Blue light (405-420nm) represents an exciting new direction in the treatment and management of acne. It has been clinically proven to kill Propionibacterium acnes and improve inflammatory acne. The great advantage of this treatment is that it has no side effects so is ideal for those who have found pharmaceutical therapy problematic.

Ambicare Health market the leading home blue light device called Lustre Pure Light. It was developed by a number of leading UK scientists and dermatologists and delivers the safe, visible part of the blue light spectrum at 420nm. The Lustre Pure Light Pro device is designed to be used for 20 minutes every day. When used as recommended it delivers a total dose of 42j/cm2 of blue light per week.
In our clinic, we conducted a trial using Lustre blue light with patients ranging from 16 to 58. The group was split into those that used only blue light for their acne and those that used blue light in conjunction with topical products (Obagi Clenziderm). All participants had facial acne ranging from mild to moderately severe.
Participants were evaluated at week 7 and week 12 for clinical improvement. They were extensively photographed and their comments and reflections were filmed.
All participants at week 7 noticed an improvement in their inflammatory lesions, comedones and the general appearance of their skin. At week 7 those on combination treatment (Clenziderm and blue light) showed the most significant improvements. At week 12 all participants had noticed significant improvements in their acne measured by a reduction in inflammatory lesions, reduction in comedones count and reduction in seborrhea.
Objectively, all participants experienced significant improvements in their facial acne at week 12 regardless of which treatment group they belonged to.
If you want to read more, the experts at Consulting Room really know what they're talking about and have put together some scarring, acne, specialist skin creme and Obagi FAQs just for you.
If you have more questions, you can use the acne, scarring, specialist skin creme and Obagi question feature to talk to our panel of trained medical experts.
If you're keen to get started with acne treatment right away then you're in luck - those clever folks also have a list of trusted, accredited acne and scarring, specialist skin creme and Obagi in your area.
It's so easy to do, you'll barely have any time to say goodbye to your acne!
Many thanks to the author Dr Johanna Ward who is An award-winning Cosmetic Doctor and GP with a special interest in clinical dermatology and nutrition. She studied English at Oxford University before studying Medicine at Guys, Kings and St Thomas’ in London.
Dr. Johanna is an advanced cosmetic injector and laser practitioner as well as training other doctors nationally and internationally. She is often called up in the media to comment about all things aging, dermatology and nutrition-related. She is the author of the best-selling book ‘Superfoods to Superhealth’ and is currently the resident skin doctor for Women’s Health Magazine.

There are many ways that menopause can affect the skin. Let's talk to an expert...
From facials, to peels, to tweakments - we ask the experts how to get the bro glow…
If your skin is ageing faster than your mind, we hear you, and so does the Morpheus8 treatment...
Hey, wait!
Before you go.....
Let's stay in touch, pop your details here and we'll send our editor's hand-picked updates on your fave subjects.